AIR LEAK SYNDROMES
Types of air leaks
Patients “at-risk” for air leaks
Signs of air leaks
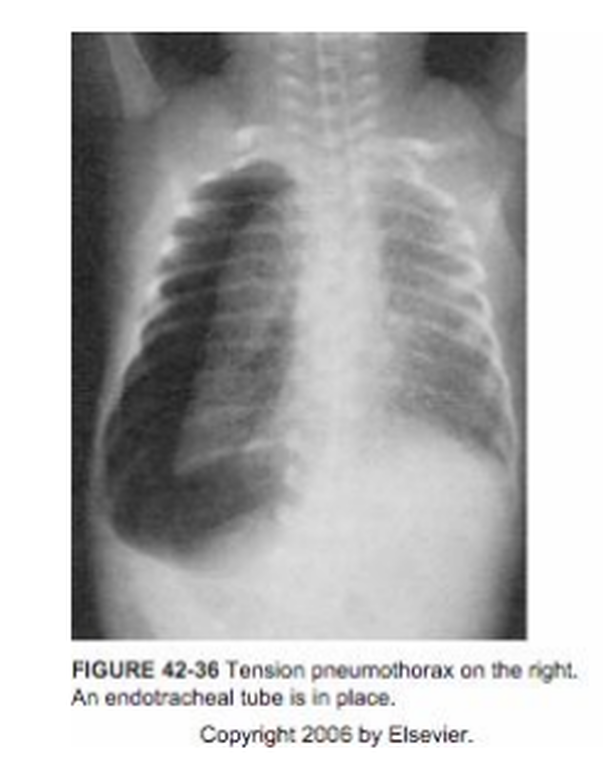
Tension pneumothorax - leads to acute moderate-to-severe deterioration in most patients.
Types of air leaks
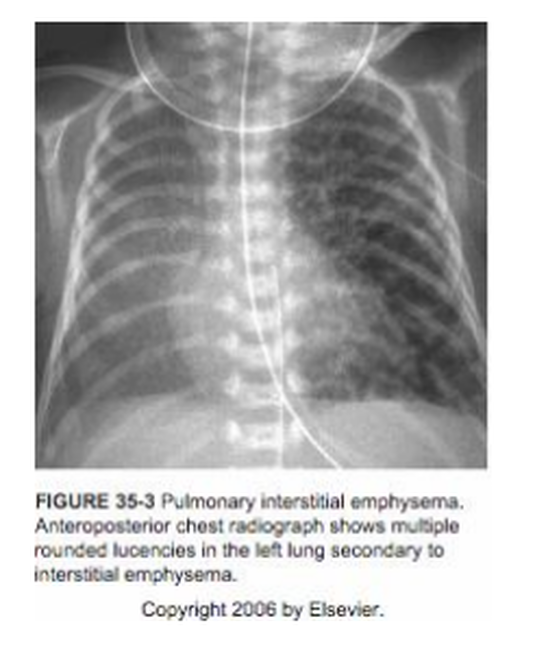
- Pulmonary interstitial emphysema (air dissects along bronchovascular bundles)
- Pneumomediastinum (rarely requires therapy)
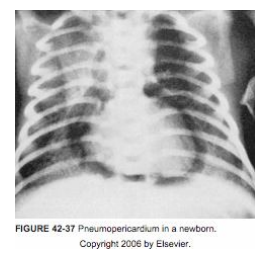
- Pneumopericardium (rare but frequently fatal)
- Subpulmonic bleb (“loculated air”)
- Pneumothorax (tension vs. non-tension) - about 1% of infants have spontaneous pneumothorax following vaginal delivery. Obviously, most of these are asymptomatic (although some infants may be tachypneic secondary to pain)
Patients “at-risk” for air leaks
- Receiving positive pressure ventilation or bag-mask-resuscitation
- Immediately after giving surfactant (which results in rapid changes in lung compliance)
- Aspiration syndrome (blood, amniotic fluid, meconium)
- Pulmonary hypoplasia
- Inadvertent placement of ET tube (i.e., right mainstem intubation). Patients with one type of air leak are capable of developing other types (PIE may lead to pneumothorax, etc.)
Signs of air leaks
Tension pneumothorax - leads to acute moderate-to-severe deterioration in most patients.
- Deterioration of blood gases (increasing PaCO2 and decreasing PaO2)
- Decreased air entry (decreased chest movement with each breath)
- Displaced PMI
- Decreased blood pressure & perfusion leading to a mottled appearance
- Tachycardia followed by Bradycardia – as venous blood return continues to be impeded, cardiac function becomes more impaired (potentially leading to cardiac arrest)
- Abdominal distension
- Decreased QRS voltage
- Mediastinal shift by X-ray (but may be misleading in presence of stiff lungs)
- Tachypnea
- Asymmetric chest wall movement when head is in midline position
- Asymmetry of transillumination of the chest wall
Pneumopericardium
- Decreased cardiac output & poor atrial filling resulting in poor perfusion
- Decreased pulse pressure
- Distant heart sounds
- Decreased QRS voltage on EKG
Pulmonary Interstitial Emphysema
- Deteriorating blood gases
- Increasing O2 requirement
- Almost always seen in preterm infants who frequently - but not always - are on higher than normal vent pressure settings